How I Do It: Teaching the AAC Helpers

 We welcome Amanda Samperi back to these pages with more ideas for prAACtical ways to address AAC implementation challenges. As an SLP, Amanda has served individuals with complex communication needs in school, home, and medical settings. She has presented on AAC-related topics st ASHA, an IEE Electrical Safety Workshop, and at the AAC in the Cloud Conference. Amanda hopes to continue sharing her knowledge and experiences about AAC through her blog, AAC is where it’s AT. Today, she shares some ideas for helping staff members better support AAC learners.
We welcome Amanda Samperi back to these pages with more ideas for prAACtical ways to address AAC implementation challenges. As an SLP, Amanda has served individuals with complex communication needs in school, home, and medical settings. She has presented on AAC-related topics st ASHA, an IEE Electrical Safety Workshop, and at the AAC in the Cloud Conference. Amanda hopes to continue sharing her knowledge and experiences about AAC through her blog, AAC is where it’s AT. Today, she shares some ideas for helping staff members better support AAC learners.
::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::::
How I Do It: Teaching the Helpers

Mr. Rogers had it right – you will always find people helping. Helpers make our world go round. We rely on them in times of tragedy, celebrate with them in times of joy, and lean on them in times of need. Helpers play a large role in both the home and school lives of children. At home, helpers include grandparents, aunts/uncles, cousins, friends, neighbors, baby sitters, and other members of the community. At school, helpers include teaching assistants, nursing staff, volunteers, and anyone else interacting with our students.
It takes a village of helpers to raise a child. But, how do we help these helpers to better interact with users of AAC?
Teach the Helpers
As professionals and experts in the field of AAC, it’s our job to train others. Without instruction and explanation, helpers will likely make decisions or follow instructions that are well-meant, but may not be in the best interest of the person using AAC.
But… there is SO MUCH information! Where to start?
Teaching wait time (count to 10)
AAC is far more laborious and time-consuming than typical verbal speech. Also, the executive functioning demands are enormous when using AAC. Just think about it – You have to follow the conversation, establish to communication partners that you have something to say (to have time to create your message), develop the message in your head and maintain that while navigating through the AAC device, locate 1 or more icons to make a message, access the device correctly, and fix any potential errors. That’s a lot! Additionally, individuals that use AAC have a variety of diagnoses, some of which impair processing time and/or response time, which can make the process even longer.
My motto: count to 10 in your head.
Maintain eye contact, and wait. This allows for the individual to have a chance to go through the process of formulating a response. It will feel like forever, but it’s worth the wait.
Here’s a great article from AssistiveWare about teaching additional wait time strategies, especially to peers and siblings.
What to expect when working with AAC
Every individual is different. Every user of AAC is also different.
It’s important that anyone working with users of AAC understand what to expect when working with him/her. Find a method for training that works for you! I recommend a paper that can be used as a reference throughout the year. It’s helpful to make sure you review the important stuff! Try including:
- Communication methods
- Example: I use my eyes to access a special device mounted to my wheelchair. I giggle and smile when I’m happy, and look away when I don’t like something. I’ll raise my hand if I have something to say – please wait for me to take my turn!
- Equipment maintenance
- How is the device charged?
- Is there a backup battery?
- Where is the backup charger (because there will be a day when the device comes in almost dead and the charger is at home)?
- How can the device be cleaned?
- What to do when something goes wrong
- How can I reboot the device?
- Are there common errors that I can fix easily? (Some high-tech devices come with a quick reference guide for problem-solving typical errors)
Here’s an example of back-to-school 1-sheet information from Building AAC. This can be modified to fit the needs of a communication device.
Editing
When it comes to editing devices, it’s critical that team members are on the same page! It’s vital that we come to an agreement between family, teachers, and SLP who will be responsible for editing those “in the moment” words and phrases. On my teams, we discuss a variety of editing issues that come up, like adding personally relevant vocabulary, including family and friend names. Some other important things to consider are:
- For specific fringe vocabulary that may not be applicable more than once, think about using a descriptive teaching model to describe a concept using high frequency and core vocabulary words.
- e. Instead of asking “
- This article has wonderful examples of utilizing the descriptive teaching method.
- Before adding phrases, check for the search feature to find out if the word is already there!
- Use a combination of phrase-based, individual words, and traditional orthography to design the best system for the individual
- Show individual motor pathway to new vocabulary, especially if there is more than one route
- e.g., You can find “chicken fingers” by going to “groups -> food -> meals -> chicken nuggets”
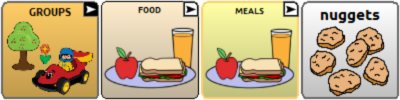 OR you can go to “eat-> meals -> chicken nuggets”
OR you can go to “eat-> meals -> chicken nuggets”
- e.g., You can find “chicken fingers” by going to “groups -> food -> meals -> chicken nuggets”
- Discuss motor planning and why it’s so important!
- I try to emphasize that I am not protective of editing the device because I think I’m the AAC Czar! Rather, someone much smarter and wiser than us put that button there for a reason. It usually has to do with the location of that button on other pages, or in relation to other buttons on the page.
- Also, related moving the symbols on someone’s device to shuffling all the apps on your phone. It would be challenging to find what you needed to find!
- Teaching others how to – and how NOT to – edit the device
How to make this happen?
In a school setting, the most efficient and effective way to make change happen is SUPPORT! It is critical to have the support of the administration in order to make communication a school-wide focus.
With support from administration comes time and resources for professional development with staff. Could you have 10 minutes at the beginning of a staff meeting to speak with the group? Meet with classrooms once a month before or after school for 15 minutes? Any time focused on collaboration is time well spent.
I also find it beneficial to work directly with support staff and teachers during AAC therapy. As I do push-in therapy in the school setting, I try to build in therapy time during small group work. That way, I get to see the students in smaller, more focused groups. Also, I get to show the support personnel on how to incorporate aided language stimulation into their academics! I get time to show what I’m expecting to be done and explain why it’s so important. It also gives the staff a chance to implement suggested strategies with in-the-moment feedback from me! I really feel that this has made my therapeutic suggestions more realistic and collaborative across the board.
Lastly, staff and parent training can and should be written into the IEP. It can be difficult to start if this isn’t something your school district is used to doing. However, it’s very important because ensures that training time is actually happening. Check out this article from Dr. Carole Zangari on more information about AAC parent and staff training in the IEP.
It takes a team to make AAC work. Find a way to help your helpers.
:::::::::::::::::::::::::::::::::::::::::::::::::::
Thank you, Amanda, for this prAACtical series!
Filed under: Featured Posts, PrAACtical Thinking
Tagged With: AAC partner training, AAC teams, collaboration
This post was written by Carole Zangari





1 Comment
Super good, thanks.